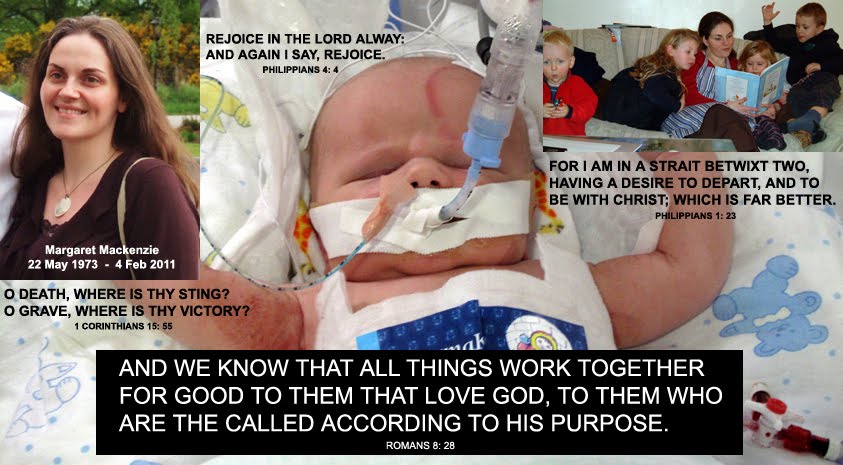
Calum Mackenzie was born at 1.59am on the 4th February 2011. His mother Margaret died just over four hours later at 6.20am. She was 37 years old. She was my wife for just over 12 years. Calum suffered severe oxygen starvation and it was touch and go whether he would survive. This blog will record his progress. Calum has 4 siblings (ages at time of writing): Jane 11; Mark 10; Sarah 8; Paul 6.
Monday 17 October 2011
Saturday 4 June 2011
Friday 8 April 2011
Tuesday 8 March 2011
St. John’s Hospital, Livingston, 3 February 2011.
We arrived in good time for Margaret’s 10.30am appointment. After arriving with her at her bed space in the ward I walked back to the car for her bags. One of them was rather heavy. When I got back to the bed I dumped the bags on the floor and told her that I wasn’t looking forward to heaving them along the extremely long corridors again after the birth and asked her what on earth she had in it. “Oh, that’ll be the one with the water bottles,” she said. Margaret left no stone unturned.
She had been admitted to hospital to be induced into labour because she was more than a week over her due date. She always wanted me to be with her during labour and birth and this time was no exception. As I sat by her bed we talked about how long the labour might be and when it might start. A midwife had given Margaret a relatively new type of treatment device called a pessary which was supposed to bring on the labour process.
We sat for a number of hours with nothing happening. During this time a midwife had been popping in to check on Margaret’s progress. Margaret was getting a bit frustrated with the delay. I told her that I had found a cafeteria upstairs and suggested that we could go there for a coffee to help break the monotony. The cafeteria was spacious with soft seating. Medical staff on breaks relaxed here and there. We sat and spoke about little things. It was relaxing and nice – a nice memory. After a while we went back to the ward and continued with our wait. Presently, a second midwife poked her head through the curtain. She was a bigger, heftier woman than the first one, with an altogether more relaxed and blasé attitude. She began to talk with Margaret. Margaret told her that the first midwife had said that the baby’s head was now down in the pelvis. “Oh, well, let’s see then shall we,” she said. She then began what looked to me like an overly heavy-handed examination of Margaret. Heaving her belly around and pushing quite roughly from side to side, saying: “No it’s not, I can move the head from side to side, see?”
I was surprised and concerned and when she’d gone I said to Margaret, “Boy, she fairly gets stuck in, doesn’t she? No messing around with her.”
I had witnessed Margaret being examined by various people during her pregnancies and they had always been very gentle, but this one surprised me with her heavy-handedness.
Afterwards I went upstairs to the canteen for a meal and when I returned Margaret told me that the first midwife had been back at her bedside. Margaret had told her what the second midwife had said. The first midwife’s response was: “Yes, because she knocked it out!” (The baby's head.)
As the hours slowly passed, I wiled away the time by jotting down thoughts in preparation for the sermon I was due to preach to my fellow students at the Faith Mission Bible College the next morning. Margaret thought that I ought to excuse myself from it due to the birth. I knew the college would accept this excuse, but I wanted to be present to preach if I could. I made it plain to her that I would only do it if it was comfortably possible. Otherwise I was absolutely willing to stay with Margaret for the duration. I would only preach if the window of opportunity allowed. Then it would be over and done with, and I could once again concentrate on Margaret.
Since 5pm (after the heavy-handed midwife had examined her) Margaret had been complaining about unusual abdominal pains. She kept mentioning it and she was worried about it. This went on for hours. I didn’t understand at the time, I thought it was just one of those strange pregnancy feelings and didn’t suspect anything serious.
It was something serious – she was hemorrhaging.
This would be Margaret’s fifth birth and she kept saying that she had never experienced pains like this before. She said she knew that they weren’t labour pains.
Eventually the night-shift midwives came on shift. At this point, I noticed a marked change in staff attitude. This time the midwife who stood at the end of the bed seemed to be determined to keep Margaret at a distance. Margaret was acutely aware of this, and kept saying to me things like: “They’re trying to fob me off – they just want an easy time – they want you to go home and me to go to sleep just so they can have an easy time of it.” At one point (about 9pm) Margaret asked the same midwife if she would examine her. It was like pulling teeth. The midwife’s response was to sigh patronisingly, and talk to Margaret as if she was some annoying child, telling her that in three-and-a-half hours – three-and-a-half hours mind you – she was due an examination and to just wait till then. But Margaret wasn’t to be put off that easily, and told the woman that she felt she needed to be examined now, and wanted to be examined now. The midwife sighed again, “Oh, all right then.” looked at her watch and said, “I’ve got a couple of things to do first. I’ll come and examine you in an hour or so.”
The next time I saw that midwife was at ten o’clock, when she told me that I had to leave. Home was a half-hour drive away in Edinburgh.
This to Margaret was unprecedented. She had never heard of a husband being asked to leave while labour was being induced. Certainly I have no memory of it happening before. Margaret was very unhappy about this and asked the midwife why I had to go. She replied: “The rules state that the partner can only stay if you’re actually in the delivery room.”
It seems stupid, considering they were trying to induce labour, which could have started at any moment, at which point they would have immediately moved us to the delivery room.
Margaret was very unhappy with the attitude of the midwives and with her treatment. The very sad and ironic thing about all of this is that she had at one point years before, expressed an interest in nursing. And midwifery is something she would have excelled at. Anyone who knew Margaret would agree that no one would have been more caring, dedicated, willing and professional than her. Had the roles been reversed she would have bent over backwards to accommodate every whim of the patient – nothing would have been too much – that’s how she lived – serving others and always more than willing to serve.
Even though I was prepared to stay and sit at her bedside for as long as she wanted me to, the thought of getting a good night’s sleep in my own bed before preaching in the morning wasn’t unappealing. And after all, I had been told that I had to go. Anyway, they would call me if things started happening.
Little did I realise the storm that was about to break upon me.
Margaret was very unhappy about me leaving. I kissed her goodnight and went home. It was the last time I saw her alive.
The phone woke me from a deep sleep at 2am. Immediately I thought it was the hospital and that the birth must have started. I grabbed the phone.
“Is that Mr Mackenzie?”
“Yes.”
“We think you’d better come. Your wife has had a very bad bleed; a very bad bleed.”
Panic gripped me. “What? I, I’m coming right away!”
I couldn’t hang up the phone fast enough. The drive to the hospital was tortuous. Driving and praying that they would be okay, but ultimately saying: “they’re in thy hands oh Lord – thou knowest my desire.” I was totally in the dark as to what was actually happening.
When I arrived at the hospital, the first thing I was told was that Margaret had collapsed and had been rushed to theatre where the baby had been immediately delivered by emergency caesarean section. This, I was told had to be done, for both baby and mother’s sake. I was also told things weren’t looking good. Being told the latter by medical professionals is very ominous. My worry deepened. I was then asked if I would like to see the baby.
When I first looked at him he could have been dead. Just lying there, limp and apparently lifeless. They told me that he was “floppy”. This is the medical term used for babies who have suffered severe oxygen starvation and as a result are unconscious and unresponsive.
It was hard looking at him. I thought he would probably die, or at best be brain-damaged. Every time I looked at him, his mother and what we were currently going through filled my mind. I had to look away.
While I was upstairs with the baby I was introduced to a junior doctor as “the one who found Margaret.” The man himself then immediately re-emphasized that to me by making a similar statement: “Yes, I was the first on the scene, I was the one who found your wife.” I do not claim to remember the wording to perfection, but there can be no mistaking the message I understood: I was left with the clear impression – Margaret had collapsed and was found unconscious on the floor. The word “collapsed” was used a number of times.
I was terrified and braced for the worst for Margaret. At one point I was told that they had managed to stabilize her heart. Hope! I immediately began to plan what I was going to say to her when she regained consciousness. Something like: “Oh boy, you had us worried.” Before describing to her what had happened.
But the next update I was given informed me that her heart had become unstable again and that they had had to “open her up again.”
Earlier during this ordeal I had tried to telephone those of Margaret’s brothers and sisters who I thought might feasibly make it to the hospital. William, the eldest of her brothers was the only one I managed to contact and could make it. He was with me for some hours leading up to Margaret’s death. I was very glad of that.
Not very long after receiving this latest piece of bad news, at about 6.20am, the door opened and a very sombre group of about half-a-dozen or so blue-gowned surgeons and other theatre staff walked in. Earlier, the same group had entered in the same manner to tell me that they were doing everything in their power to save Margaret’s life. But this time the senior surgeon placed his hand on my shoulder and said: “I’m very sorry, I’m afraid she’s died.”
I broke down.
They sat in silence around the room, with long faces, looking at me. They plainly felt sorry for me. But I then felt sorry for them.
Very quickly the realization of Margaret’s happy spiritual state came before my mind and also a concern about the souls of the medical team whose attention I had at this critical moment. I was then able to compose myself and say: “Well, she’s in heaven now, and far happier than she could ever be in this world.”
A relatively small but I would not say insignificant witness. I felt that I would have liked to have said more, but Christ’s power is infinite and he is able to bless a single word. I wondered while I spoke how many of them might be atheists. I believe that God sends us these situations to be used to his glory in witnessing for the truth before our fellow sinners – “in season, out of season.”
William had also broken down at the news. He now asked me if I would mind if he phoned around the other members of the family to inform them. “Please do, I would be grateful if you did that,” I said (Margaret was one of 12 brothers and 8 sisters). I sat in silence listening to him call them and his parents one by one, his voice breaking with emotion on every call.
A nurse came in and asked us if we’d like to view Margaret’s body. We said that we would.
My body felt like it weighed a ton as I walked towards that room.
At first sight of Margaret’s lifeless face I was tempted momentarily with the thought: “poor Margaret.” But immediately faith pushed it out and replaced it with: “No, not poor Margaret, but rich, wonderfully happy Margaret, in heaven, rejoicing in the presence of her Lord.” The next thought which came powerfully before my mind was: “This is not Margaret. Margaret is in heaven – she is not here. This is just her dead body – dust.” Yes that dust is united to Christ until the resurrection, but until then she is absent.
I turned to William and said, “I don’t want to spend any more time here. There’s no point in hanging around. This is not Margaret – she’s in heaven and the baby’s been moved to another hospital – so there’s nothing here for us – let’s go.” William agreed and afterwards told me that he had been thinking the same.
As was always the case, for the duration of the birth, we had one or more of Margaret’s sisters stay in the house to look after the kids. On this night we had Johan and Flora. When William was making his calls I told him to tell the girls in the house not to tell the kids what had happened, but that I would tell them when I got home.
When we entered the house, the kids were all up and about and they seemed to be acting relatively normally, but I believe they must have suspected something as one glance at their aunties betrayed the fact that they had been crying.
I told them I had something to tell them and assembled the four of them on a couch, two on either side of me and said, “You know how mum was in hospital having a baby? Well, she had a baby boy, but I’m afraid she died.” I broke down again. Both girls burst into tears. The two boys just sat looking stunned. The aunties cried. I managed to compose myself to an extent and told them: “But she’s in heaven now, and very, very happy, and that’s what we have to remember, but we’ll miss her.”
------------------------
I have three questions: the first question is about the heavy-handed examination. This examination was performed not long before 5pm, which is the time Margaret began to feel the unusual abdominal pains (internal bleeding). The question is: did this examination cause a possibly already weakened area to actually rupture?
The second question is: if I was introduced to a doctor as the one who "found" Margaret, why was I then later given a detailed formal description (quite some time later) of the situation as: Margaret "sitting on the bed, having her blood-pressure taken by a midwife when she passed out"? There is plainly a contradiction here.
The third question is: had I had been allowed to stay at Margaret's side instead of being instructed to leave (I was in no one's way and would have been an asset, as I would have been keeping an eye on her and so would have noticed anything unusual about her and would have raised the alarm much earlier) would things have turned out differently?
Saturday 5 March 2011
Wednesday 23 February 2011
Tuesday 22 February 2011
Saturday 19 February 2011
Friday 18 February 2011
Monday 14 February 2011
Saturday 12 February 2011
Friday 11 February 2011
Thursday 10 February 2011
Wednesday 9 February 2011
Tuesday 8 February 2011


